
|
Overview
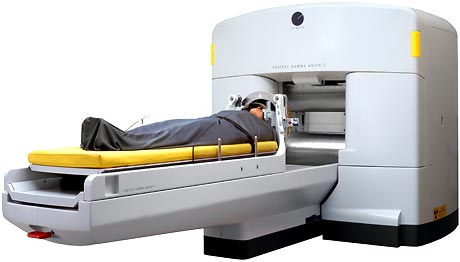
The fact is, the Gamma Knife is not really a knife at all, but a non-invasive tool that replaces the scalpel with a focused array of 201 intersecting beams of high-intensity gamma radiation.
|
|

|
The Gamma Knife concept originated in Stockholm in 1951, when Dr. Lars Leksell, a prominent neurosurgeon, coined the term "Radiosurgery."
Dr. Leksell was a pioneer in "Stereotaxy," a procedure which allows the neurosurgeon to locate and reach any point of the brain to within a single millimeter of accuracy, using trigonometry to navigate the brain's 3-dimensional space.
Consequently, in lieu of performing open surgery on the brain, the neurosurgeon has the ability to precisely focus gamma radiation on a target tumor or vascular malformation.
|
Focused radiation may also be used to treat "functional" disorders such as the tremors resulting from Parkinson's disease, and the pain syndrome of trigeminal neuralgia.
Contrary to conventional radiation therapy, which must be delivered in small fractions over time (often over as many as six weeks), and in which normal brain tissue may be exposed to approximately the same amount of radiation as the tumor target, Gamma Knife radiosurgery employs a greater number of lower level radiation sources (201) arranged in a collimator Helmet. The radiation oncologist and neurosurgeon intersects these beams on the target.
Each beam is very weak, passing through an area of the brain different from all of the other beams. Thus each beam is safe to normal brain tissue but where they focus is 200 times as powerful as each individual beam.
|
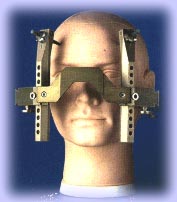
How the Beams are Directed
|
|
In order to focus the beams precisely and accurately, the patient must be fitted with a painless "stereotactic frame" prior to the MRI and Gamma Knife procedure.
The combined effect at the intersection of the beams is 201 times as powerful as each individual beam, and can obliterate tumors and vascular malformations in a single treatment.
Gamma Knife radiosurgery is not experimental. The first Gamma Knife treatment was in Sweden in 1968, and since then nearly 75,000 patients have been treated successfully worldwide.
Gamma Knife radiosurgery has been performed on American soil for about 14 years.
|
The medical literature is replete with hundreds of articles relating to Gamma Knife Radiosurgery. It is considered the "gold standard" of radiosurgical technique. There have been no reported cases of radiation- induced cancers from Gamma Knife treatment. In a recent RTOG multicenter study, reported at the November, 1998 meeting of the American Society of Therapeutic and Radiation Oncologists (ASTRO), the Gamma Knife was found to be 3 times more likely to control brain tumors than LINAC based systems.
The Patient's Experience During a Typical Gamma Knife Procedure
The Gamma Knife treatment is usually performed in a single morning.
There is no pain, no noise (other than the MRI) and patients are invited to bring music of their choice for listening during the treatment. They usually may return to work the next day, or fly home on an airplane. There are no incisions, or sutures. The patient will usually be discharged that afternoon or if necessary, discharged on the following day. Almost all insurance company HMOs, PPOs, Medicare, Medical, etc. cover the cost of the procedure.
|
|
The typical day is as follows:
|
|
6:30-7:30:
|
Pre-op preparation
|
|
7:30-7:45:
|
Stereotactic frame application (under twilight sedation)
|
|
8:00-9:00:
|
MRI for targeting
|
|
9:00-10:00:
|
Computer Planning
|
|
10:00-11:00:
|
Gamma Knife treatment (depending on pathology, from 10 to 90 minutes)
|
|
12:00:
|
Stereotactic frame is removed and Patient returns to the hospital room or is discharged.
|
|
A More Detailed Day
|
|
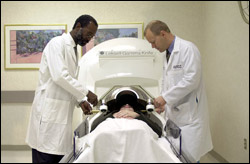
Dr. Phillip St. Louis, neurosurgeon, and
Dr. Mike Sombeck, radiation oncologist,
preparing a patient for radiosurgery.
|
|

|

|
|







